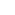Treatment
The information below is the result of observations and experiences of the ZARD community. Due to limited research on symptom management and treatment guidelines, the Foundation hopes to bring value by highlighting this anecdotal evidence along with symptoms noted in clinical research. For published research please click here.
All medical treatment plans, including risks and benefits, should be thoroughly discussed with the patient’s medical team as each patient is unique.
If you are a parent and/ or patient affected with ZARD and wish to share your own observations and experiences, we encourage you to contact us at connect@zc4h2foundation.org.
Symptom management and clinical treatment of ZARD may involve the following medical specialties:
The primary care provider coordinates multispecialty care for the patient along with chronic and acute health management. The pediatrician is essential especially during early childhood development when consults to specialists are initiated. Many families agree the first couple of years are the most challenging due to navigating all the specialists and consults required for our medically complex patients.
Many patients are born with contractures at birth often diagnosed as arthrogryposis. Patients are also followed for feet deformities, hip dysplasia, and scoliosis. Most children with ZARD will need one or more orthopedic surgical interventions, the most common being feet and knee corrections, spinal surgery, and hip surgery.
An important observation from our community is the worsening of range of motion after surgery. This may point to the impaired remodeling/healing of soft tissue in our condition. As we do not yet understand the physiology of muscle and soft tissue in ZARD patients, we strongly recommend discussing invasive surgical interventions at length, seeking second opinions, and whenever possible and safe, considering conservative approaches such as serial casting, bracing and therapy.
Further research to the physiology and function of muscles from ZARD patients will hopefully offer further insights.
The surgical outcomes from spinal fusions including growth rods have been largely positive. Hip surgeries have mixed outcomes, so a patient centered approach as it relates to quality of life is best. Patients have often noted concerns with surgical outcomes regarding knee contractures. Serial casting, bracing, and physiotherapy have shown to give positive results generally. Serial casting is best when done in early childhood. Ponseti method for clubfoot correction has been a best practice in our patients.
It is important to note that some patients can have diagnosed spasticity. These patients generally respond well to Botox and phenol injections.
Most patients benefit from custom orthopedic bracing including AFOs, wrist splints, and in some cases KAFOs and HKAFOs.
ZARD patients, like many AMC patients, seem to have a predisposition to respiratory problems postoperatively.
All patients with ZARD are officially diagnosed through genetic testing. Worldwide, the diagnostic testing protocols vary greatly. Some newly diagnosed patients’ families have experienced frustration with lack of information about ZARD. This is very common and the Foundation is working diligently to help geneticists empower their patients with up to date and relevant information. Appropriate genetic counseling is crucial, especially in the early stages after diagnosis.
Current published research can be found here
Neuromuscular symptoms are a characteristic in many patients. This can include spasticity, dystonia, apraxia, and neuropathic pain. Many patients, depending on their presentation, may benefit from drugs such as baclofen or gabapentin. Some patients have reported issues with autonomic nervous system dysfunction including flushing. Some patients have been diagnosed with epilepsy. Your neurologist should recommend the most appropriate approach to monitoring any possible abnormal activity. For more complex cases it may be helpful to consult an epileptologist.
Brain MRIs have not been a strong indicator for neurological impairment in our community since brain structure in the majority of patients appears normal or with certain variations of undetermined significance.
Breathing issues are not uncommon with ZARD patients especially at birth. Fortunately, many patients outgrow these challenges. Some patients have been treated successfully for aspiration pneumonia through (prophylactic) use of antibiotics for example, azithromycin. Patients have benefited from nebulizers, chest percussion therapy, postural drainage, and supplemental oxygen. Some patients require a gastric tube and fundoplication due to aspiration while swallowing. In rare cases patients benefit from tracheotomies. Medical treatment during respiratory illness is strongly encouraged to prevent possible complications.
In most cases, especially the first year of life, timely and periodical swallow studies have been necessary to determine the appropriate protocol for management of aspiration pneumonia in ZARD children.
Pneumonia in ZARD is often a secondary infection. The primary issue in ZARD is motor planning impairment, which affects the coordination of breathing and swallowing. This leads to micro and macro aspirations, increasing the risk of respiratory complications. During seasonal viral infections, postnasal drip worsens due to excess mucus and fluids in the throat, further impairing swallowing and breathing coordination. This in turn increases aspiration, which can result in secondary bacterial lung infections. However, children with ZARD typically do not have compromised immune systems or excessive saliva production.
Key Recommendations: 1. Recognize the root cause: Respiratory issues in ZARD stem from aspiration caused by motor planning deficits. 2. Interventions: • Preverbal speech and feeding therapy with specialists in oral motor therapy or apraxia to improve safe swallowing. • Long-term prophylactic azithromycin • RSV vaccination: as RSV increases secretions for prolonged periods, and therefore the risks of aspiration, it often leads to bacterial pneumonia in ZARD. (Our knowledge and community experience is limited to the antibody-type vaccines for RSV. For other type of RSV vaccines, please discuss with the treating physician).
Understanding these factors can help doctors and caregivers prevent and manage pneumonia effectively.
Physical Therapy, including early intervention, is one of the crucial supportive approaches for ZARD. Some young patients in early intervention (0-3 years) have seen success with a neuro development approach to physical therapy. Usually, this approach focuses on minimizing reflexes or integrating them into functional movement. Some patients report spasticity categorized as mixed muscle tone combined with motor apraxia. Tight abductors and hamstrings as well as muscle atrophy has been reported in many patients.
The Foundation encourages PTs to take a patient centered approach and focus on independent mobility as opposed to walking when appropriate. Massage that focuses on neurological pathways can be very helpful. Tummy time is challenging for many patients, and using an exercise ball is a great way to strengthen the upper body when tummy time on a mat is too challenging for child. Caution should be taken with our children during range of movement. Some patients have reported fractures so extra caution should be taken.
Occupational Therapy is important to support the achievement and conservation of functions that pertain the day-to-day deployment of activities in children and patients with ZARD. Some of our children present with hand and finger deformities and benefit from splinting of the hands. Some fingers have “symphalangia,” meaning the finger joints are not there, or other problems of the finger joints, which can be challenging when working on fine motor skills. Motor apraxia and spasticity is especially challenging for many patients.
Impairment in motor planning -a common characteristic among ZARD patients- is the most important factor for speech difficulties seen in our children. It is important that parents and medical professionals understand that early intervention is vital to protect a child’s airway, eating by mouth, and speaking. Children with ZARD improve the best and respond the best to oral motor therapy.
Based on the experience of families with ZARD, we highly recommend speech language therapists use at least one of these three methods which should be known by a trained apraxia specialist: TalkTools, PROMPT, and Kaufman Method. It is worth searching for a speech therapist with this training or a willingness to be trained. The first two techniques use tactile input to build muscle awareness, stability, and memory for the right positions and sequences, and the third uses successive approximations. The Foundation strongly advocates for every patient with ZC4H2 to have a voice in their life, and the form that it takes will differ based on individual abilities. Patients may benefit from augmentative communication devices or need extra time to communicate.
TalkTools® Oral Placement Therapy (OPT™) is a hands-on, tactile approach to speech therapy that uses specialized tools (like straws, horns, and bite blocks) to provide direct sensory feedback to the mouth muscles. Unlike regular speech therapy, which relies mainly on listening, watching, and imitating sounds, TalkTools adds touch-based cues to help children feel exactly where their tongue, lips, and jaw should go.
PROMPT® (Prompts for Restructuring Oral Muscular Phonetic Targets) is a tactile- kinesthetic, evidence-based speech therapy method where therapists use hands on, gentle, and strategic touch cues on a patient’s face, lips, jaw, and under the chin to guide muscle movements for speech production. It is used to treat speech disorders, including childhood apraxia, autism, and articulation issues, by improving muscular control and creating new, precise neural pathways for speech.
The Kaufman Speech to Language Protocol (K-SLP™), often called the Kaufman Method, uses successive approximations (shaping) to simplify complex words into easier, child-friendly versions based on natural phonological processes starting with what the child can already produce (e.g., “nana” for “banana”) and gradually shaping toward the full adult form through repetition, cueing, and fading techniques. Unlike regular speech therapy, which often focuses on direct imitation of correct sounds/words using auditory and visual cues (listen, watch, repeat), the Kaufman Method prioritizes building functional communication first by targeting simplified word approximations that reduce motor planning demands. The method provides repeated successful practice, builds motor memory and confidence, reduces errors, and prevents frustration which allows faster gains in consistent, functional speech production when traditional imitation-based methods alone lead to limited progress or increased struggle.
In the first few years of life, many children with ZARD also struggle with oral feeding or have difficulties coordinating breathing and swallowing, either by anatomical malformations (such as laryngomalacia or cleft palate) or by impairment in the oral motor planning, or both. This can lead to (recurrent) aspiration pneumonia. Some outgrow those challenges and learn to eat and drink by mouth. Others benefit from gastric tubes for nutrition and may taste foods for pleasure as opposed to full nutrition. A swallow study is often helpful prior to feeding patients when concern is warranted based on medical history. The goal should be overall wellness of the child in terms of nutrition so an individual approach is recommended based on ability.
Some patients have been diagnosed with cortical visual impairment, a visual/ neurological processing issue, and/ or ocular apraxia, including Duane syndrome. Issues with the physical structure of the eye are limited, but a few patients have been diagnosed with ptosis, strabismus, exotropia and/ or underdeveloped ocular nerve.
Feeding and breathing issues seen in our children, especially in the early years, may have diverse reasons; either anatomical malformations (such as laryngomalacia and jaw deformities) or neurological causes like the broadly reported difficulties to coordinate breathing and swallowing at the same time, which may be a consequence of motor planning impairments. Other symptoms as apnea and Eustachian tube disfunctions have been reported too.
All patients with ZARD should be screened for tethered cord through MRI. Multiple patients have been diagnosed with tethered cord over the last years. Before surgery involving the spine including fusions or baclofen pumps, tethered cord should be thoroughly ruled out to prevent long term complications. Occult tethered cords have also been reported. MRI should be performed at a children’s hospital that routinely performs untethering procedures for most accurate results. Tethered cord surgeries have been successful and life changing in some patients.
A few patients, mainly males, have cardiac heart defects and/or heart rhythm disturbances.
Some patients have experienced issues with blood sugar levels. Hypoglycemia or other abnormal glycemic responses have been reported.
Most children can be overweight and have big appetites. We don’t really know the endocrinologic reason behind it although there are indications of insulin resistance in some children. Some patients present premature adrenarche and/or early puberty. Patients in many cases have shown improvements with diet modification including a diet based in restricted calories and carbohydrates. A regimented or continuous feeding schedule has been helpful and a few children have needed medicine to control hyperinsulinemia.
Some patients, especially those suffering from spasticity and discomfort, have benefited from phenol injections and Botox. Phenol injections are directed at the nerve as opposed to the muscle like more commonly used Botox. Phenol injections are performed under anesthesia usually by a physiatrist or orthopedic surgeon. Cases of baclofen pump trial are very limited at this time, but tethered cord should be thoroughly ruled out before attempting pump.
The Foundation strongly encourages all surgeries to be completed at a reputable children’s hospital with a pediatric anesthesiologist experienced with complex cases. ZARD patients can have issues with breathing and heart rate during procedures which is routinely treated with proper care and precautions. Patients should be monitored closely in the pediatric intensive care unit due to breathing complications after anesthesia. Some patients have remained intubated longer than usual for the safety of the patient’s airways. Some patients have shown sensitivity to medications that suppress the respiratory system (such as opioids) and should be well monitored.
Many ZARD patients have difficulties for venipuncture, with veins difficult to localize. In some cases, access for intubation has been reported to be challenging.
The orpha.net publication, Anesthesia recommendations for patients suffering from Arthrogryposis multiplex congenita – June 2011 (orpha.net) has been helpful to both patients and providers. The foundation encourages its distribution to the surgical team before any procedure especially time-intensive surgeries.
Understanding and Treating Constipation
Constipation is a common challenge with patients with ZARD. Physical activity and diet modifications can be helpful, but it is common for a parent to try all the typical advice given by their pediatrician and still encounter challenges with their child not pooping regularly.
A normal daily bowel movement is healthy and necessary to prevent serious issues. These educational videos in English and Spanish, explain the process of having a bowel movement and the challenges that occur with constipation. A person suffering from constipation needs two types of medications to have a healthy pain-free bowel movement. A medicine that softens and a medicine that helps you push out the poo. To soften the poo, polyethylene glycol is commonly used and an alternative is magnesium. To push out the poo, senna is an ideal choice. Finding the correct dosage and combination is often achieved through trial and error. Glycerin suppositories are helpful when the person has been holding, due to prolonged sitting and inability to get to a toilet or a comfortable position for pooping. Simply insert, and it should produce a bowel movement within minutes. Unlike an enema, glycerin suppositories are not messy and rarely cause cramping. The Bristol Stool Chart is a simple picture guide that shows 7 types of poop to help parents and doctors talk easily about a child’s bowel movements. The goal is usually to aim for Type 3 or Type 4, a sausage shape that’s either a bit cracked on the surface (Type 3) or smooth and soft like a snake (Type 4). These types are the healthiest and easiest to pass without straining or pain.
Probiotics or fermented foods are recommended for all patients including those dealing with digestive issues like constipation.
Constipation, though a sometimes-embarrassing topic should be taken seriously. It can cause pain and discomfort along with hemorrhoids and anal fissures. The lack of a normal bowel movement can also lead to further digestive issues including but not limited to reflux, slow gut motility, visceral hyperalgesia (difficult to treat, consistent pain), small intestinal bacterial overgrowth, and hospitalization due to impaction. Constipation is especially challenging post-surgery so discuss with your team prior to surgery and how to alleviate issues in the hospital before discharge.
Constipation and Gastroesophageal Reflux Disease (GERD)
Constipation can contribute to or worsen GERD and acid reflux symptoms, though the relationship is often bidirectional or overlapping rather than purely one-way causation.
Reasons include:
- Increased intra-abdominal pressure– Straining during bowel movements (common in constipation) raises pressure in the abdomen, which can push stomach contents upward through the lower esophageal sphincter (LES), promoting reflux and triggering heartburn or regurgitation.
- Shared motility disorders– Both conditions can stem from broader GI motility issues. This includes slowed movement throughout the digestive tract due to nerve/muscle problems and enteric nervous system dysfunction. The enteric nervous system (ENS) is a complex network of over 100 million neurons embedded within the walls of your GI tract, from the esophagus to the rectum. It operates largely independently of the central nervous system (brain and spinal cord) while still communicating bidirectionally with it via pathways like the vagus nerve. This forms part of the gut-brain axis.
- Slowed or delayed gastric emptying and overall GI slowdown– Constipation is linked to prolonged transit in parts of the upper GI tract in some cases, allowing more time for acid production or reflux.
- Medication overlap– Some treatments for GERD (certain proton pump inhibitors or antacids) can cause or contribute to constipation as a side effect, creating a cycle. The reason PPIs can cause constipation isn’t fully clear but may relate to changes in gut motility, microbiome alterations, or direct effects on intestinal function with acid suppression. Alternatively, magnesium-based antacids can cause a laxative effect.
- Other factors including bloating from constipation, inactivity, or visceral hypersensitivity– Visceral hypersensitivity (also called visceral hyperalgesia) is a condition where the internal organs, particularly in the GI tract, become overly sensitive to normal sensations that most people wouldn’t notice or find painful. In simple terms, it’s like the “volume” on gut sensations is turned up too high. Everyday processes like digestion, gas movement, mild distension (stretching) of the intestines, or even eating/drinking can trigger amplified signals of pain, discomfort, bloating, urgency, or cramping that get sent to the brain and interpreted as significant issues. This heightened sensitivity occurs because the nerves in the gut (part of the enteric nervous system) lower their threshold for detecting and transmitting pain signals. Normal gut activity that should feel neutral or barely noticeable becomes exaggerated, leading to symptoms that feel disproportionate to what’s actually happening in the body. Consider the treatment of gabapentin if this is a concern. Click here for more on pain assessment and treatment.
Scenarios where correcting constipation likely won’t provide relief include: GERD without concurrent constipation, structural or anatomical causes of GERD, underlying motility disorders beyond simple functional constipation, and/ or non-reflux related symptoms mimicking GERD (like food allergies). In these cases, additional testing is recommended.
Enteral Nutrition: Gastric (G) tubes, Nasal Gastric (NG) tubes, and Jejunostomy (J) Tubes
Children with ZARD have feeding tubes placed if they cannot successfully gain the skills to safely eat due to motor planning issues (see treatment section on speech language pathology). A G tube may be placed as an infant and ideally, years later as a result of proper oral motor planning therapy, the child will transition to oral nutrition. We do not recommend the use of nasal gastric tubes except in the hospital for acute reasons like short term illness. NG tubes in babies can be harmful when oral motor planning concerns are taken into consideration. These primarily involve oral aversion, food refusal, feeding tube dependency, delayed transition to oral feeds, and altered oral sensitivity, issues that interfere with learning and practicing coordinated sucking, swallowing, and eating. In ZARD, long-term NG tube use (often beyond a few weeks to 3 months) can reduce positive oral experiences during critical developmental windows, cause negative sensory stimulation from the tube (e.g., irritation or discomfort), and limit practice of natural swallowing patterns. If enteral nutrition is required for an extended period of time, we recommend placing a G tube and removing it when the child no longer needs it. The removal typically does not require surgery and closes naturally. We do not recommend that a child be discharged from the hospital with a NG tube.
Diet and Feeding Challenges
Patients with ZARD can be overweight, especially females. This is more evident in late infancy or around puberty. However, in early infancy, weight tends to be lower than average, for both girls and boys. How ZARD affects metabolism is not yet understood. A diet of healthy, real food, low carbohydrates, low sugar, and plenty of water is very important for healthy weight, also in ZARD. For patients on enteral nutrition, whole food formula or a blended diet is ideal and recommended.
As previously commented, feeding challenges (aspirations) are common in early infancy in ZARD. Thickening agents for liquids can offer a safer way to oral feeding and have been successfully used for feeding of ZARD children. Small bites of food -versus watery food like apple sauce- are recommended by parents who successfully trained their children to eat safely.
When choosing what to feed your child, remember that the core issue in ZARD is impairment in oral motor planning, which causes difficulties in the coordination of swallowing and breathing, resulting in (silent) aspirations and choking. We recommend parents and caregivers instruct themselves on how to perform the Heimlich maneuver or have an anti-choking device for emergencies.
Limited verbal communication, communication delays, fixation on certain activities and objects, and motor planning issues have been reported. Autism has been diagnosed in patients with ZARD. Additional research is needed to form a more accurate picture of these behavioral differences in the ZARD community. Cognitive evaluations are often inconclusive because the standard tests require motor planning and mobility to respond. Many of our children are in general education classes with individual supports as needed. The Foundation encourages inclusion in the school setting.
Wheelchairs, standers including mobile standers, and/ or gait trainers are utilized by ZARD patients. Mobility independence is important for all children including ZARD patients. Some patients love their adaptive bikes, which can help with range of motion and prevent further contractures, but should be used in caution with patients susceptible to fractures. All terrain wheelchairs, beach wheelchairs, adaptive sleds, and jogging strollers are mobility devices that encourage inclusion and bring joy to our loved ones with ZC4H2 Associated Rare Disorders.
Pain is a common and severe issue for patients with central nervous system impairments, including ZARD, especially those with significant disabilities. With better understanding and tools, pain can be more effectively recognized and managed, even with challenges like identifying pain, limited medication experience, or treatment hesitancy. Dr. Julie Hauer’s insightful paper, Pain Assessment and Treatment in Children With Significant Impairment of the Central Nervous System, explores neuropathic pain, pain behaviors (including in nonverbal patients), muscle spasticity, chronic pain sources, and pain management. It includes the WHO’s 1986 analgesic ladder to guide medication selection and highlights gabapentin’s role in treating neuropathic pain (Table 7). We invite you to share this valuable resource with your physician to support collaborative care, especially in teaching hospitals. For a deeper dive, view the Pediatric Grand Rounds lecture on chronic neuro-pain in children with severe neurological impairments.
For a parent-friendly guide, visit Managing Pain in Children with Complex Chronic Conditions – Courageous Parents Network (in English and Spanish).
The guide includes recognizing the following common distress behaviors:
Muscle tensing or tightening at intervals: increased spasticity, stiffening of legs, drawing up arms, clenched fists, tremors or jerks, tense and still, kicking, thrashing
Change in body position: back arching, rigid and stiff, head movement, thrashing
Change in facial expression: grimace, frown, clenched jaw, distressed look, eyes wide open, or non-expressive face
Change in vocalizations: crying, soft moaning, grunting, gasping
Change in interaction: withdrawn, less active
Skin changes: pale or flushed skin, sweating
Can’t be calmed: efforts to comfort the child don’t seem to ease the symptom
Additionally, Dr. Hauer’s book, Caring for Children Who Have Severe Neurological Impairment: A Life with Grace, is a compassionate resource for parents of children with severe ZARD. We hope these resources empower you to advocate for improved pain management for your loved ones with ZARD.





ZC4H2 Research Foundation, Inc. All rights reserved.
ZC4H2 Research Foundation has been recognized by the Internal Revenue Service as a 501(c)(3) organization. EIN: 87-4577599